Hopefully this series of blogs will answer the many questions that cancer patients and the public are asking about how Ian Gawler might have been misdiagnosed?
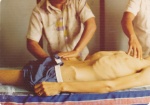
After all, we would normally think of TB being associated with a ‘shadow’ on the lung, not large calcified lumps such as the those photographed on July 7 1977 – Ian’s chest wall…(below left).
In my next blog we will look at how misdiagnosis can happen and how TB can mimic even bone cancer. The following will form a background and framework for what has happened and make sense of this complex story.

I was once quoted as saying “I would rather be married to a live anecdote than a dead statistic.” At that stage I had no idea that our story would become so famous and that people would try to emulate what we did throughout the course of Ian’s illness. I had neither the maturity nor expertise to tease apart various medical incidents that had always left me wondering.
Now in 2012, having walked in the world of cancer medicine for 38 years; by logic, you would have to think that I have seen a thing or two! Add to that my experience as sole caregiver/partner for Ian Gawler throughout his illness; first in 1974 as girlfriend when he was diagnosed with osteogenic sarcoma; then supporting him throughout his assumed recurrence; marrying him when he’d been given a few weeks to live, and following through with support until he returned to full health. Given that background, you would have to think that I know a thing or two!
Coming back to current time, Ian Gawler and supporters mistakenly believe they are at war with the medical profession who are simply out to discredit because he recovered from secondary bone cancer despite them. This debate has reached the heights of blind emotionalism fanned by Gawler’s blogs calling it the Spanish Inquisition! Rather than welcoming enquiry, the Gawler Foundation has published links to these emotive blogs on their front page! Has anyone from this group stopped for moment to consider why, as an ex wife I would expose myself to public and medical scrutiny by correcting errors of fact about Ian Gawler’s ‘remission’ in a medical journal? We separated long ago – so although it makes for exciting press, there are no duelling Mrs Gawler’s as has been implied. I have been preoccupied since 1997 with a medical condition myself and family responsibilities, so could well do without the hassle. We should also ask why two eminent professors of oncology would risk their reputations publically and medically by investigating Ian Gawler’s recovery 30 years on? Bringing a tone of logic to the matter, it is recommended that Ian Gawler’s supporters read the evidence as written in the IMJ report before making assumptions about wars and conspiracies. Haines and Lowenthal’s report is well written and scientifically intelligent and for me who was intimately involved in Ian Gawler’s recovery; in 2012 ‘science-speak’ – it sure makes a lot of sense!
We must remember that medicine was a very different entity in the 1970’s. Sophisticated scanning wasn’t around and diagnostics were perhaps more dependent on the patient’s reporting of symptoms. There were very few medical practitioners involved in Ian Gawler’s case; they were not of long duration and, as well, we had much geographical relocation during his illness. No one picked up the symptoms of TB, no one knew of the BCG vaccines he had used as immune stimulants and no one knew of the tuberculin he used for TB testing cows in veterinary practice in those days. No one asked if indeed there had been a biopsy performed 11 months after amputation when a bony lump appeared in his groin. No one asked about biopsies for the duration of his illness; it was presumed they had been done. Maybe this assumption was due to the fact that Ian Gawler was a Veterinarian who would know these things. In a nutshell, this is how much of his story/history, simply passed under the medical radar without questions and eventually became a well reported ‘anecdotal cure.’
When Ainslie Meares reported Ian’s story in 1978 in the MJA – there was one missing piece to the puzzle – Meares did not know Ian had been diagnosed with advanced TB in June 1978. Meares had written and submitted the abstract when the calcifications on Ian’s Chest disappeared – he too presumed the growths had been metastatic cancer – in the absence of knowledge about Ian’s TB. He also inverted Ian’s medical timeline which has helped fuel the current confusion in terms of what happened when?
The ‘Dragon’s Blessing’, Ian’s biography was published October 2008. Dr Alistair Robertson is quoted in the book. He had reviewed Ian Gawler’s case in 1978 and made the diagnosis of TB. This was the first time Ian had consulted him, so he had little or no background about the case. He looked at x-rays from previous years; back to 1976 and compared them with the current-time June 1978 films. Robertson said: “TB had been evident for at least two years” however, the lung ‘shadow’ was evident early in 1976 on x-ray. I remember asking Ian’s radiation oncologist about it in February 1976 but I had never seen TB; as a veterinary nurse in wasn’t in my repertoire.
Enter the MJA “True Stories” December 2008 – a 30-year follow up report about Ian’s survival. Authored by Ian’s GP wife Ruth and his work colleague George Jelinek, the report was not only flawed with reversed timelines, inaccurate dates including original dates removed from photographic material relating to key parts of Ian’s medical history, but there was also a ‘not true element’ such as the vegan diet Ian never had that formed a part of their conclusion as to why he recovered! A lot was left wanting and it is incomprehensible that the report had been published without adequate fact checking.
Then, September 2010 my MJA Corrections letter was accepted and published after almost a year of fact checking. The Gawler/Jelinek 2008 MJA “True Stories” resembled nothing of the story I had been involved with from 1974 – 1978. Gawler/Jelinek’s response in the MJA was obscure with little relevance to my corrections. Again they questioned the date of the famous chest wall photographs; I was wrong they said. However as well as having originals with dates that correlated with my corrections, Ian Gawler’s You Can Conquer Cancer had already reproduced 250,000 copies of the photographs with the date that was the same as mine!
Gawler & Jelinek had stated that Ian Gawler developed TB in 1978 and then it was treated by conventional drugs. Had they read Ian Gawler’s biography released just a couple of months before their MJA, they would have seen Dr Alistair Robertson’s comment about ‘concurrent disease’ and the thought that it may have had something to do with his remission.
It seems my corrections letter had opened a can of worms. TB was clearly becoming an important and contentious element in the morphing of the Gawler ‘remission’ story. There is no mention of TB in all reprints and editions of You Can Conquer Cancer, Meares 1978 abstract and many other publications.
Then to my surprise and amazement, Haines and Lowenthal had checked in with information available on the public record and began to join the ‘tubercular dots’ which formed the basis of their 2012 IMJ Hypothesis. With additional knowledge that were no biopsies of Ian Gawler’s ‘metastatic’ disease; they could make a much more plausible assessment of his medical condition.
Despite media hype and reporting, paradoxically, much of Ian Gawler’s medical history and timeline had remained wrapped in a cocoon of silence because no one had asked the question! Haines and Lowenthal finally asked the question and came up with some scientifically plausible answers. They say it all in the conclusion to their paper:
This hypothesis is advanced for two reasons. The first is to underline the modern recognition of the need to consider diagnostic investigations, including biopsy, before assigning the diagnosis of advanced cancer to any patient. This principle is especially vital in cases where two diseases can present in the same way. The second is that there a risk that if diseases are incorrectly labelled, incorrect treatments may be given. This can lead to misleading interpretations being made about non-traditional treatments providing “cures,” which can influence the decision-making of patients seeking answers and even lead them away from potentially curative traditional treatments.
For more see: www.https://theconversation.edu.au/coffee-enemas-dont-cure-cancer-reviewing-the-remarkable-claims-of-ian-gawler-5242